ILC's Treatment for Lumbar Compression Fracture
Having been adopted in over 54 countries globally,
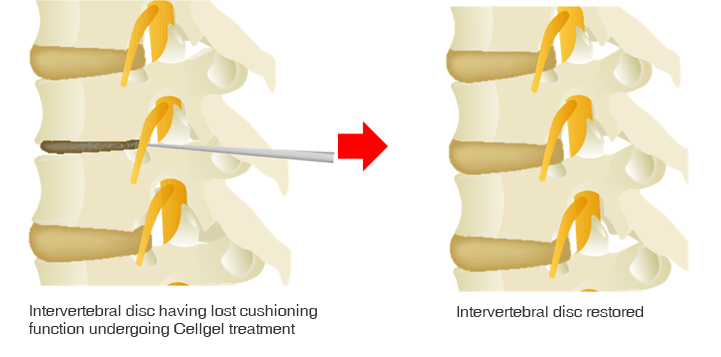
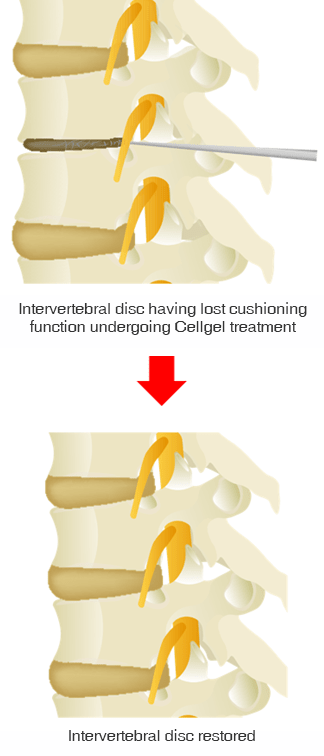
the "Cellgel Method" for treating lower back pain
is now available in Japan
For those who have been told it was impossible to operate,
For those who have had recurrence of pain post-surgery,
A low-risk, outpatient treatment is now an option for you.
Contents
 Table of Contents
Table of Contents
- 1 What is lumbar compression fracture?
- 2 Main symptoms of lumbar compression fracture
- 3 Causes of lumbar compression fracture
- 4 Why is the recurrence rate so high?
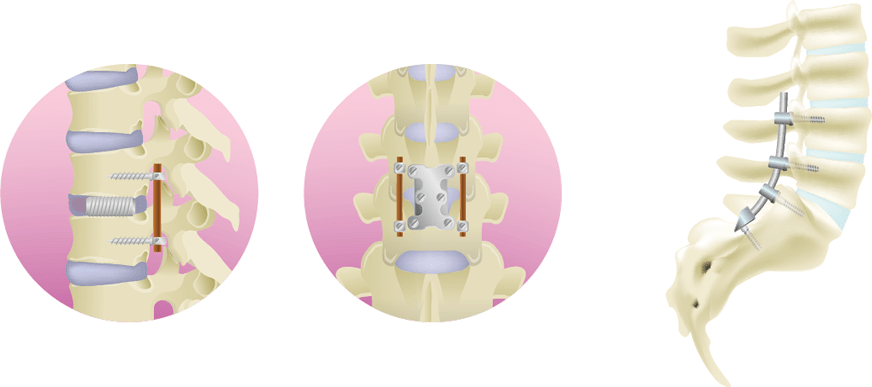
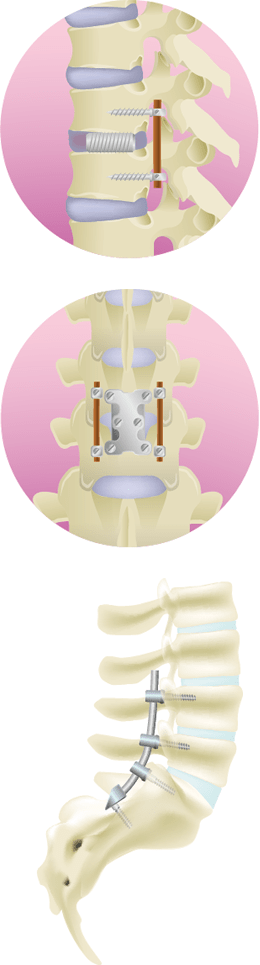
- 5 What are the effective treatments for lumbar compression fracture?
- 6 Treatment at ILC
- 7 FAQ about lumbar compression fracture and treatment
This page provides information on the main symptoms and causes of lumbar compression fracture and our treatment procedures. The information includes the method of treatment, treatment time, and information about insurance. We use the Cellgel method, which is one of the most advanced methods in the world, and the characteristics of this method are also described in detail.
Please read this page especially if you have been told that you cannot be cured without surgery, if you have had surgery in the past but have not improved, or if you got better after surgery but the symptoms have recurred.
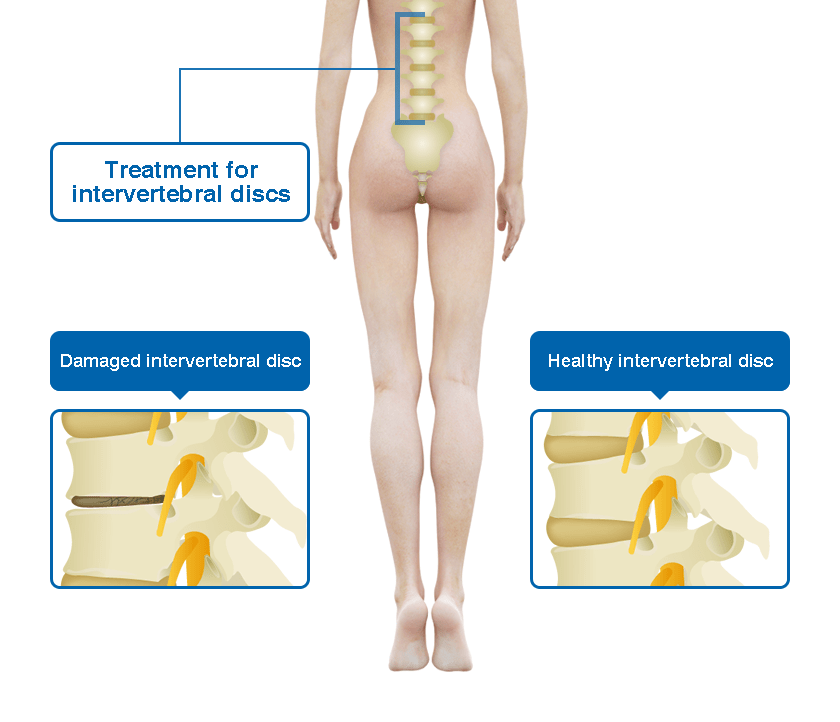
What is lumbar compression fracture?
A compression fracture is the collapse of the vertebral body in the spine. If it occurs in the thoracic spine, it is a thoracic compression fracture; if it occurs in the lumbar spine, it is a lumbar compression fracture. Compression fractures occur at a rate of 10.8% in men and 22.2% in women in their 70s, with approximately 300,000 to 1 million new cases reported.
A lumbar compression fracture is a fracture caused by a vertical force. Characteristically, it is more common in postmenopausal women, and in the early stages, many complain of pain every time they move their bodies.
In younger people, fractures are rarely caused by minor external stresses, although they can be caused by strong impacts such as falls from heights or traffic accidents. As people get older, they are more likely to develop osteoporosis (brittle bones), a condition in which bone strength decreases. As osteoporosis progresses, lumbar compression fractures may occur when the body is unable to bear the weight of the body due to buttocks or normal daily activities (twisting at the waist, carrying heavy objects, etc.).
As stated by the Orthopaedic Society, a person who has had one fracture of the spine is four times more likely to have a new spinal fracture. Femoral neck fractures (fracture of the bone at the base of the thigh) are also known to be almost twice as likely to occur.
The key to healing a lumbar vertebra compression fracture is how well the fracture site is kept at rest.
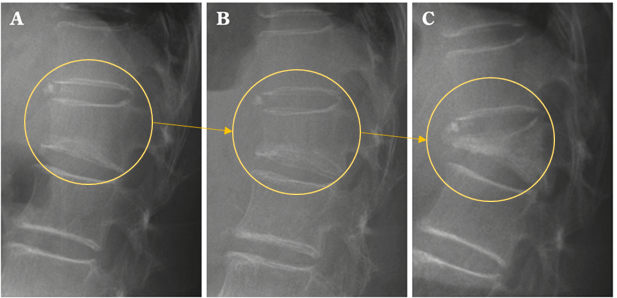
Immediately after the injury, the fracture site is extremely unstable, and as shown in the radiograph below, vertebral deformity can develop.
Progressive vertebral deformity can lead to prolonged pain and a loss of alignment of the spine itself.
*Reference for image: Research Article "Treatment of Osteoporotic Lumbar Compression Fractures" (https://www.jstage.jst.go.jp/article/jcns/25/9/25_718/_pdf)
Main symptoms of lumbar compression fracture
The main symptom of a lumbar compression fracture is localized lumbar pain. If the fracture is complicated by the condition of the fracture or spinal canal stenosis, it may be accompanied by nerve-related problems such as leg pain and numbness.
The intensity of symptoms varies greatly from person to person, with some patients experiencing pain so severe that they cannot walk and others experiencing only a mild dull ache.
Chronic pain may vary daily in terms of intensity, but if the pain is severe, the patient may not be able to turn over in bed or move the body from a sleeping position to a sitting position.
If the patient continues to forcibly move the body to avoid pain, or to keep the fracture in a posture that compresses the fracture, the fracture will worsen and the pain will be prolonged.
The vertebral body (spine) that has been fractured by a compression fracture will not return to its original state, and the bones will fuse in a deformed state, leading to:
- i. Chronic lower back pain
- ii. Spinal kyphosis (hunched back, making it difficult to straighten the spine)
- iii. Higher likelihood of falls due to poor posture
- iv. Decline in overal quality of life
If you have any of these symptoms, we recommend that have it checked as soon as possible.
Causes of lumbar compression fracture
Lumbar compression fractures may be caused by:
- 1. Osteoporosis: Bone density decreases and the vertebrae cannot withstand the compression force, resulting in a fracture.
- 2. Trauma: Lumbar compression fracture is caused by a strong external impact to the vertebrae due to a fall or traffic accident.
- 3. Pathological fracture: The strength of the vertebrae is reduced due to bone tumors, etc., and the vertebrae become vulnerable to fracture.
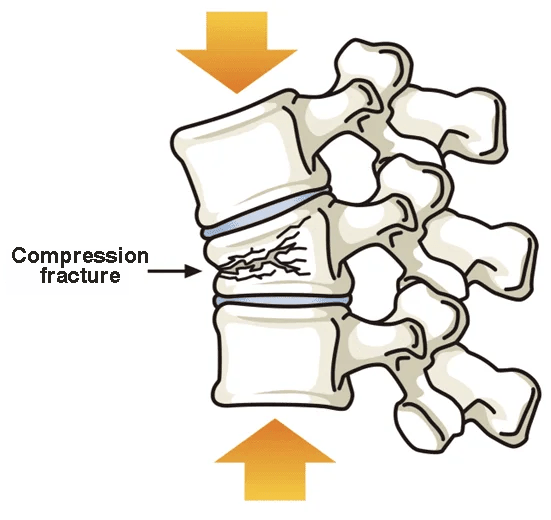
Why is the recurrence rate so high?
Once a lumbar compression fracture is sustained, the incidence of compression fractures of other vertebrae is said to increase. It has been reported that the probability of a compression fracture in one vertebra is 2.4 times higher than that of a person without a compression fracture in the five years following the injury, and 4.9 times higher if there are two or more compression fractures.
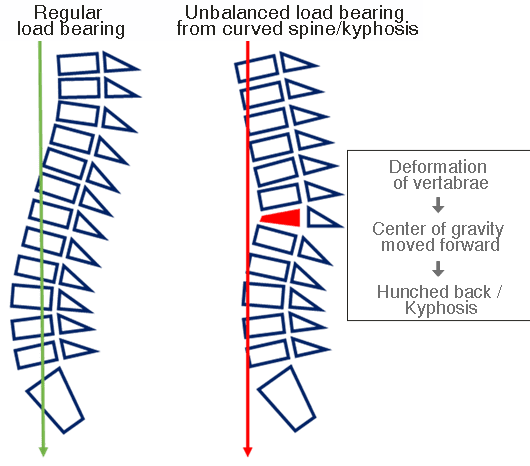
This is due to the fact that once a compression fracture is sustained, the standing posture becomes hunched, and when the back becomes rounded, the center of gravity is displaced forward. As the center of gravity moves forward, the spine continues to experience compressive forces, triggering compression fractures in other vertebrae.
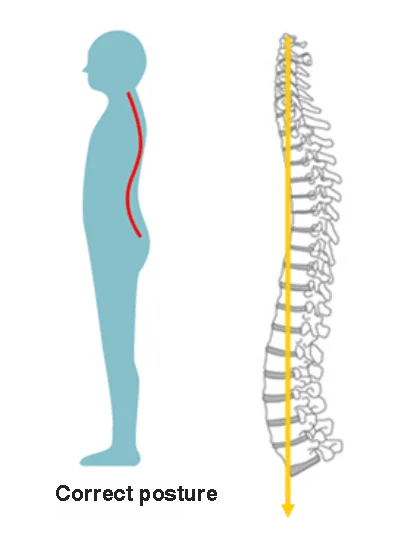
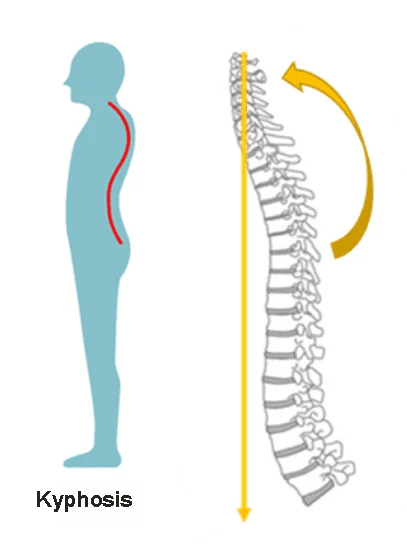
In addition, once a compression fracture of the spine occurs, the intervertebral discs above and below the fractured bone can degenerate, leading to herniated discs and spinal canal stenosis. The images below are actual patient cases reported in the paper.
Degeneration of the intervertebral discs increases the risk of not only herniated discs and spinal canal stenosis, but also changes in posture and muscle use that can lead to a variety of other problems, such as those listed in our list of spinal diseases.
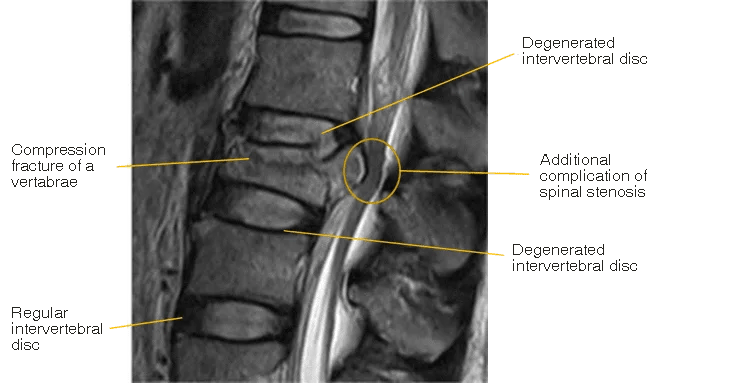
Image Reference: Thesis titled "A retrospective study evaluating the correlation between the severity of intervertebral disc injury and the anteroposteriortype of thoracolumbar vertebral fractures"